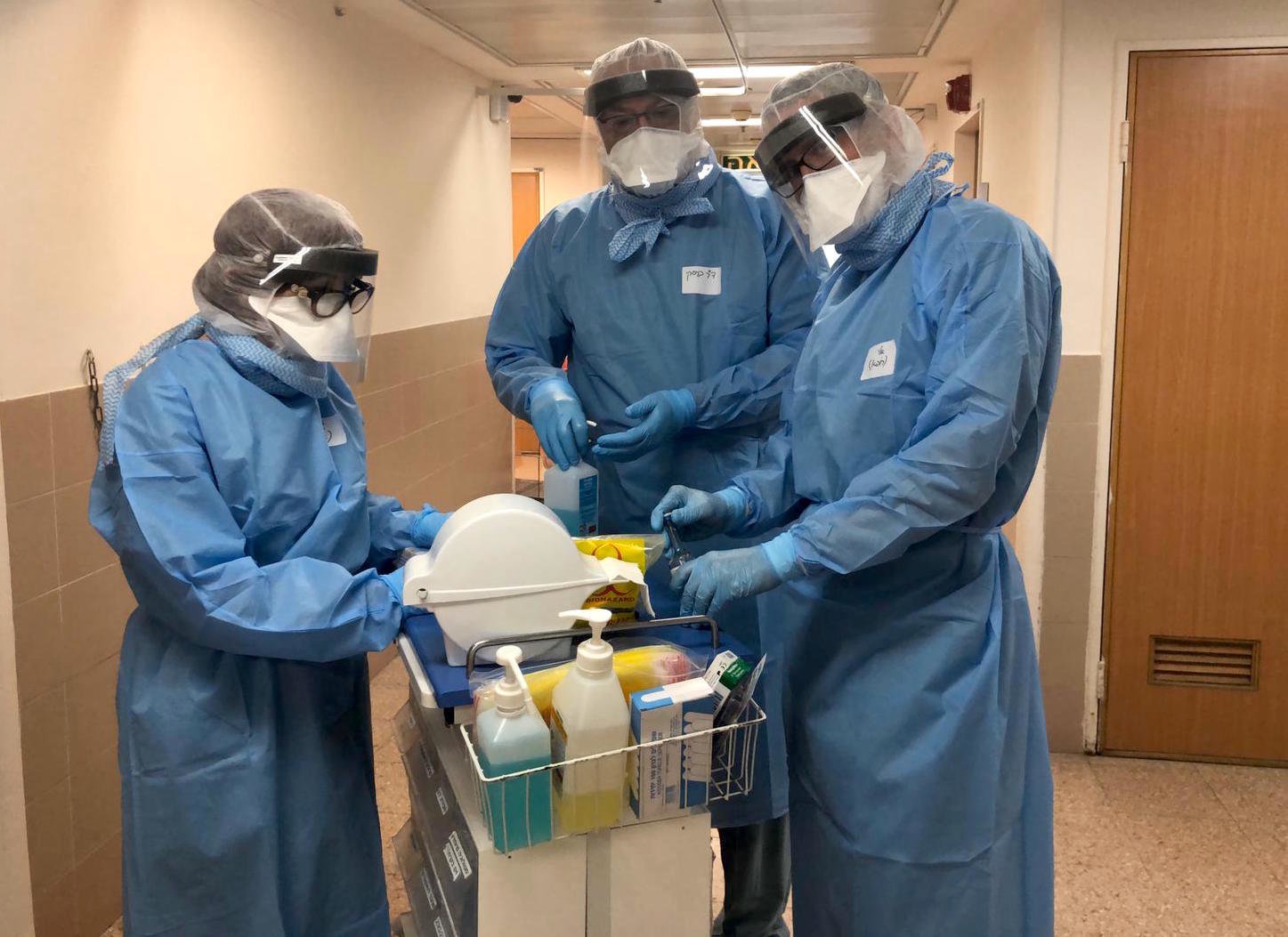
Israeli doc ready for months on the front line
When it became clear that the COVID-19 pandemic would reach Israel, Elli Rosenberg was one of a small number of medical professionals at the Soroka Medical Center in Beersheva to answer a call for volunteers to treat the sick.
Rosenberg, a clinical immunologist who works as an internist at Soroka, now runs the coronavirus unit there.
JTA: Were you prepared for this?
Rosenberg: We imagined this day might come, but never translated that into operational contingencies. Everything is new here. The last two weeks have been a learning process and a training process for something that might get much worse very quickly.
What did you do on Day 1?
When the first patient was admitted to our unit, I remember suiting up and getting into all the layers of protective gear and entering an airlock that separates the clear zone from the infected zone. It was an astronaut-like experience. As I held the door of the airlock, I felt, wow, I’m stepping into the unknown and taking part in something that’s a worldwide challenge. It was a mixture of fear and excitement and a reminder of why I chose to do what I do.
How do you provide care given the risk of contagion?
Our unit is divided into two sections: the confirmed corona section, where everyone who has the same disease can interact, and another unit for patients with high suspicion of corona where each patient is isolated in his or her room until they receive test results.
What we’re trying to do is maximize patient care with minimal staff exposure. Technology helps. A coin-sized monitor taped to their chest — developed by an Israeli startup company — continuously transmits vital signs by Bluetooth to our control center. We also have tablets for the patients that measure their temperature and can serve as a stethoscope. Students and faculty from the engineering department at Ben-Gurion University of the Negev are building a telemedicine robot to our specifications.
What is the course of treatment?
There is no evidence-based treatment yet. There’s a lot of research being carried out around the world.… We’re basing what we do on developing supportive care, usually with oxygen, and waiting for the patient’s own immune response to kick in and eliminate the virus.
How long does it typically take for patients to get through coronavirus?
Between several days and a few weeks. That’s the challenge with this disease. If there’s an influx of patients that require hospitalization for long stays, that might overwhelm the health care system’s capacity. There won’t be enough beds, there won’t be enough staff, there won’t be enough respirators.
How are the patients managing the emotional burden of isolation?
The uncertainty is very intense. Every cough, every fever, every change in their oxygen saturation level is usually a cause of a lot of stress. The cough and shortness of breath are nasty. The isolation from family is very difficult. They’re essentially locked in. Using telemedicine, they speak daily with a social worker to try to vent their feelings, their concerns, their fears.
We see every patient every day face to face even if there’s not a medical necessity for it. I think they feel much more secure when we’re in there with them. The human contact, putting a comforting hand on their shoulder, has a psychological impact.
What are the greatest risks to you and your staff?
The true front lines are the people working in emergency rooms. Any patient that walks in potentially has corona, and the staff there doesn’t have the ability to protect themselves from every single patient. That uncertainty increases the risk of accidental exposure. In our unit, there’s no uncertainty.
Do you check yourself or your staff for the virus?
No. The protocol is that as long as we feel well we’re not tested on a routine basis. If any of us develops fever or respiratory symptoms suggestive of the disease, we’ll obviously test. The consequence of positive results among any of our staff would be quarantine for everybody. And that has extensive repercussions, so we’re hoping we all stay healthy.
I have extensively limited my exposure to other wards in the hospital. I’m also limiting my exposure to places where I might contract the virus. I haven’t been in stores, I haven’t gone to shul.
What does your family say about your work?
I think they understand the importance of what I’m involved in. My 12-year-old daughter specifically pointed out that she’s proud of me, which moved me greatly.
What do you tell your family about how to stay safe?
Wash hands frequently. Don’t touch your face. Try not to come into physical contact with other people. Try to limit your distance to anybody outside of the family to about 6 feet. In my house, there have been extensive changes in dining etiquette. There’s no more drinking straight from the milk carton or sharing spoons. That’s been a major change in our household. I have been limiting myself to very little physical contact with my wife or my children.
What’s your take on Israel’s handling of the pandemic?
In the beginning, I thought this was handled way too aggressively and that the measures the government decided on were extreme. As time progressed, especially with examples coming in from different countries around the world of how governments responded and what the consequences were — for better and for worse — I slowly shifted to the point right now where I hope we’re not too late with the actions we’re taking.
How long do you think this will last, and how bad will it get?
Nobody really knows. I’m mentally preparing for a few months. I’m also preparing for a situation where it gets worse before it gets better. We’re trying to make the most out of the resources we have. Will we be overwhelmed, will we find ourselves in a similar position to what’s happening unfortunately in Italy, where doctors are making horrible choices of who to treat and who to turn away? I dread that possibility. We’re trying to do the best with what we have to avoid that situation.

 45.0°,
Partly Cloudy
45.0°,
Partly Cloudy